Management of Clubfoot in Horses: Foals to Adult.Reprinted with permission from the American Association of Equine Practitioners. |
 Fig. 1. |
| Grade 1 clubfoot. On the lateral view, note the mild flexural deformity and the heels slightly off the ground. On the dorsal view, note the lack of flare in the hoof capsule as it grows distally and the disparity in width between the coronet and the ground surface of the hoof that would indicate decreased loading. |
 Fig. 2. |
| Before and after appropriate trimming. Note the improvement in the hoof-pastern axis and the bevel (arrow) created in the solar surface of the hoof. |
3. Juvenile Presentation
The most frequently recognized form of clubfoot in horses occurs in sucklings or weanlings at approximately 2 to 8 months of age.1-3,6-8 It is commonly a unilateral condition but occasionally affects both limbs. The first clinical sign recognized is an upright appearance of the foot combined with the inability of the heels to contact the ground immediately after trimming the foot. As the condition progresses, the coronary band develops a square or full appearance dorsally. As the toe wears, the upright nature of the foot becomes more evident and the foot assumes a contracted shape, losing its flare as it grows distally (Fig. 1). The dorsal hoof wall begins to dish and widens at the white line. Concurrently,the carpus often assumes a back-of-the knee conformation. The toe may become bruised and ultimately abscess, resulting in severe lameness.Because of the abnormal forces on the distal phalanx and inflammation associated with excessive loading, bruising, and abscessation, pedal osteitis is a common occurrence.
Differentiation should be made between a developing clubfoot and a foot that is upright from excessive wear at the toe. The latter is a self-limiting problem as long as lameness is not severe or from abscessation. If lameness is present, a protective device over the toe will generally alleviate the problem once the foot grows sufficiently. A foot of this type responds well to most treatments, and undue credit is often given to aggressive therapy that was unnecessary in the first place.
Clinical management of clubfoot is influenced by the severity, duration, and the etiology of the clubfoot as well as the degree and source of lameness, if present. Evaluation of the foot should be performed at rest and in motion. The angle and balance of the foot should be determined and the foot should be inspected for under-run or separated wall or sole. Sensitivity to hoof testers or response to firm pressure from fingers should be assessed. If lameness is present, peripheral nerve blocks should be performed to isolate and confirm the origin of the lameness. Radiographs of the foot should be taken to assess the position and the integrity of the distal phalanx or presence of other pathology. If there is evidence of pedal osteitis, especially in the presence of a severe clubfoot, venographic evaluation may aid in prognostication. If the clubfoot is secondary to lameness of other origin, it is imperative to isolate and resolve the other lameness prior to attempting therapy for the clubfoot.
The shoe can be further modified to unload painful areas of the sole or if the sole has dropped or prolapsed by recessing the shoe's solar surface. Shoe modifications are easily added or subtracted (i.e. rasping the toe of the shoe to adjust breakover), with the foot in the farrier position. The wooden shoe being malleable will often be modified by normal wear which allows the horse to find a comfort zone unique to its individual needs.
Treatment in the early stages of development of clubfoot involves establishing a normal hoof angle by lowering and spreading the heels as long as the foal remains sound. One should adhere to the guidelines for trimming and providing a sound, balanced foot.14-16 The bars should be removed to decrease as much restrictive mass of the hoof capsule as possible, and the frog should be trimmed to healthy, compliant tissue to enhance loading. The wall through the quarters and heels should be lowered to the plane of the frog and parallel the frog. It has been suggested to apply a reverse wedge pad under the toe to determine the amount of heel to lower before reaching a level of discomfort of the foal.2 If the toe is worn excessively, a protective device applied to the toe to prevent bruising and subsequent lameness may be applied. The toe may be rounded, squared, or beveled to promote breakover and alleviate any lever effect of the toe as well as to reduce stress on the lamellae (Fig. 2). Toe extensions applied to provide a lever arm using a shoe or composite material are contraindicated because they may exacerbate wall separation in addition to delaying break-over. Extensions may also contribute to lameness from excessive tension of the deep digital flexor unit if the foal fully loads the foot.
 Fig. 3. |
| Lateral view of a grade 3 clubfoot. Note the flexural deformity, the disparity of hoof wall growth between toe and heel, and the concavity in the dorsal hoof wall. The palmar view shows contracted heels and the frog recessed between the hoof wall at the heels. |
In the event of lameness isolated to the foot, it may be necessary to elevate the heels to establish weight-bearing on the involved foot. Presumably this is beneficial if the pain originates from tension of the flexor apparatus. In the author's experience, heel elevation is temporarily beneficial, but attempts to resume a normal hoof angle should commence as soon as the foal is comfortable and bearing full weight. The hoof angle may be reduced gradually over a period of weeks; however, if pain recurs, the foal should be considered for surgery. Other forms of hoof appliances in common used to treat this condition include slipper shoes and spring loaded spreader shoes. These devices appear to increase the width of the distal portion of the foot; however, this occurs by shearing and separation of the laminae through the quarters, which ultimately undermines the integrity of the hoof. Actual spreading of the foot must begin from within the foot at the coronary band by increasing load through the bony column to the axial and load-bearing surfaces of the foot, with the foot properly trimmed. Application of flexible synthetic shoes, a which are nonrestrictive and allow expansion of the foot with compliant properties similar to the hoof capsule, have promise in horses that have a foot with deficient wall for sustaining load during regrowth. Other methods of obtaining expansion of the hoof include variations on resecting sections of wall through dorsal wall thinning or removal to the level of the lamina or placing multiple vertical grooves the full length of the wall. Although there is no body of evidence to substantiate the efficacy of these techniques, there are anecdotal testimonies of larger foot growth after these procedures have been performed.
A severe clubfoot is usually complicated with contracture of soft tissues surrounding the distal interphalangeal joint, including the joint capsule and presumably the collateral ligaments or other supportive structures in the region. Therefore, there are inherent limitations on the effectiveness of corrective procedures. Alleviating tension of the deep digital flexor tendon (DDFT) by transection of the DDFT accessory ligament or transection of the DDFT may not yield a normal angle of the hoof and may not produce soundness, although it is unusual not to obtain some degree of improvement with surgery.
Other alternative modalities of therapy to consider include the use of oxytetracycline (44 mg/kg,IV, SID)13 or other medications aimed at reducing tension on the DDFT tension apparatus. Theoretically, oxytetracycline produces chelation of calcium ions with the net effect of relaxation of muscle groups.17,18 Unfortunately, with clubfoot disorder having a propensity to be accompanied by back-of the-knee conformation, the drug typically worsens the carpal conformation while having limited effects on the foot. The author routinely administers oxytetracycline in conjunction with performing surgery to enhance relaxation of the muscle unit and relax other involved soft tissues. Other antimicrobials, such as enrofloxacin,b clinically produce a similar effect of relaxation of the flexor tendons and may have benefit similar to oxytetracycline. Botulinumtoxin is used in people and has been reported for use in horses with laminitis to achieve relaxation of the DDFT to prevent distal phalangeal rotation.19 With appropriate application, the drug may have merit in the management of clubfoot in horses in the future.
Clubfoot may develop in the yearling or may be a continuum of the process initiated earlier in life. In general, the older the animal is at the onset, the less likely of obtaining a normally conformed foot, although this does not necessarily preclude a successful athletic career. If the condition is acquired as a yearling, it is almost always secondary to a lameness or gait deficit resulting in inappropriate loading of the foot, such as with a neurogenic disorder. If the primary disorder is rapidly rectified, the foot may return to normal if the gait is restored to normal before the development of irreversible changes in the foot. The mechanical principles involved in therapy are the same as for the weanling, and the primary objectives with any of the procedures are to maintain comfort and to obtain a mechanically sound foot. Changes in hoof shape achieved in yearlings (and adults) are often less than those obtained in younger horses.
4. Adult Presentation and Management
Adult clubfoot disorders may be present as the result of previous clubfoot as a juvenile, may be secondary to other lameness, or may result as a sequel to chronic laminitis. The principles of management of clubfoot in the adult are the same as in other age groups; however, pathologic changes of the foot are often more advanced because of the duration of the deformity (Fig. 3). Expectations for a favorable outcome are largely determined by the following factors: the severity of the deformity, the duration the deformity has been present, the integrity of both the hoof capsule and third phalanx, and the intended use of the horse (breeding versus athlete). Many horses are able to compete athletically with a clubfoot as long as they are maintained on a consistent hoof management program.
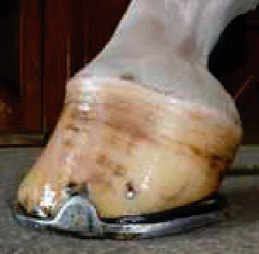 Fig. 4. |
| Clubfoot illustrated in Fig. 2 after appropriate farriery. Note the concavity in the dorsal hoof wall reduced the improvement in the hoof-pastern axis and the heel elevation necessary to load the heels. |
Mild deformities are managed in large part through routine farriery aimed at trimming for optimal and uniform load-bearing of the entire hoof wall. The hoof angle required to achieve this type of load-bearing is usually steeper than normal but is a necessary compromise to avoid lameness associated with either hyperextension of the distal interphalangeal joint and accompanying structures or excessive stress on other soft tissue structures, which often occur secondary to an attempt to establish a normal hoof angle. Break-over may be enhanced in these individuals by rolling or rockering the toe. As in the management of all clubfeet, the foot must not be allowed to grow to extremes and undergo separation of the wall. The general guiding principle is to trim the foot at an angle that allows full loading of the heels or landing flat-footed when ambulating. Mild heel elevation may be necessary to accomplish fully loading the heels. The heels should not be lowered to the point of allowing toe contact before heel contact at the walk (Fig. 4).
If the hoof wall integrity is poor and the foot undergoes recurrent bruising and abscessation, protection of the wall and sole through shoeing or casting may be necessary. Similar principles apply regarding uniform loading of the wall and enhancing break-over to reduce shear forces along the dorsal laminae, as in milder cases of clubfoot.
Adult breeding horses with a clubfoot are subject to excessive trauma at the toe and subsequently are prone to develop subsolar abscessation and eventual pedal osteitis. Extra measures in these horses may be useful, such as shoeing to protect the toe. In protracted, severe cases of clubfoot deformity with advanced pedal osteitis, desmotomy of the accessory ligament of the DDFT or DDF tenotomy may be beneficial. Desmotomy of the accessory ligament of the DDFT is usually reserved for less severe cases of clubfoot deformity in which the individual is intended for athletic endeavors. Clinical experience has yielded favorable results from these procedures in the form of improved integrity of the wall, expansion of the hoof capsule, and an angle that is closer to normal in addition to a reduction of hoof abscessation. If the decision is made to perform a deep digital flexor tenotomy, although improvement is usually achieved whether the tenotomy is performed mid-metacarpal or mid-pastern, clinical impression is that the mid-pastern tenotomy produces more relaxation of the tendon and therefore more derotation of the distal phalanx.
5. Surgical Procedures
The underlying premise supporting surgery for treatment of clubfoot is to relieve the rigid tension band of the DDFT extending from the third metacarpus via the accessory ligament of the DDFT to insert on the distal phalanx. The two methods of accomplishing this include transection of the accessory ligament of the DDFT and transection of the DDFT. Several techniques have been described to accomplish each procedure.20-24
Transection of the accessory ligament of the DDFT has been described, using conventional surgical dissection from a lateral or medial approach, using ultrasound guidance, using tenoscopic guidance,and performing the surgery in lateral or dorsal recumbency. Each technique has advantages and disadvantages; the main disadvantage all techniques attempt to avoid is the cosmetic blemish associated with the surgery. I do not believe there is a difference in cosmetic outcome with one technique over another, provided the surgery is performed proficiently and the patient is tractable for appropriate bandaging and exercise for the first 3 months after surgery. There is variation in the amount of exercise allowable, depending on the condition of the feet. With conventional surgical descriptions, a medial approach is often described; in my experience, this approach requires significantly more dissection and there is a higher likelihood of a blemish as a result. Personally, I find a blemish on the medial aspect of the limb as offensive as on the lateral.
The most straightforward technique and commonly performed technique is accomplished by using conventional surgery in lateral recumbency positioned for a lateral approach, with the affected leg up. The skin may be rolled palmarly before incising, so the final placement appears over the fourth metacarpal bone. The skin incision begins 2 cm distal to the head of the fourth metacarpal bone and extends distally 2 cm. Sharp dissection is continued through the subcutaneous tissue, the fascia of the flexor carpal sheath and paratenon, exposing the junction of the accessory (inferior check) ligament with the DDFT. A pair of curved hemostats are passed along the dorsal border of the accessory ligament and the DDFT and spread, then withdrawn. Next, the hemostats are passed along the palmar border of the ligament in a similar fashion. Care must be taken to avoid the neurovascular bundle along the medial aspect of the limb. Digital palpation of the superficial digital flexor tendon (SDFT) and DDFT is performed to confirm that the proper structure has been isolated. The lower limb may be slightly flexed to relax the ligament that is isolated, exposed, and exteriorized with the hemostatic forceps, and then transected. I generally remove a 1-cm section of the ligament, although removal of this section is not necessary, it requires more tissue dissection, and the second transecting cut can be difficult to accomplish neatly. The limb should undergo extension and flexion, and the operator should observe the movement of the structure to ensure complete transection. Interestingly, with severe clubfoot deformity, the ligament is often significantly larger than normal. Closure should be performed in three layers, being careful to leave a 0.5-cm opening in the distal portion of each layer to allow for drainage, should a seroma occur. The bandage should extend above the knee and be taped to prevent slippage and exposure of the incision. If there is no slipping of the bandage, the first bandage should remain in place 4 to 5 days before changing. The foot should be trimmed appropriately, and, if a corrective device such as a toe cap is needed, it should be applied. I routinely administer 2 to 3 days of oxytetracycline (44 mg/kg IV SID)13in addition to a nonsteroidal anti-inflammatory drug in the postoperative period to encourage loading the foot.
Deep digital flexor tenotomy may be performed for stage 2 deformities. As a general rule, even with severe deformities, I attempt correction with a check ligament desmotomy before this. Mid-metacarpalor mid-pastern tenotomy is acceptable, but greater release is achieved with a mid-pastern approach and is my preferred technique in adults that have repeat abscessation or septic osteitis of the distal phalanx. Reports vary regarding the level of success after surgical intervention. In general, soundness is achieved, but racetrack performance is decreased from that of unaffected siblings.20
6. Long-Term Management and Prognosis
Although clubfoot deformity in horses is common, there is a sparse amount of evidence-based work defining the syndrome and its management. Therapy is often empirical and based on clinical experience.The primary goal of therapy and management of any clubfoot horse is to obtain a sound horse with a normal or near-normal foot that will be maintained with routine hoof care. One important principle of clinical management is to determine if discomfort or lameness is present, and if so, to localize the source of the lameness and determine the association of the lameness to the clubfoot (primary or secondary). If the foot is improperly loaded, a normal-contour hoof capsule will not be possible to obtain and the underlying lameness may be the limiting factor on the future athletic capacity.